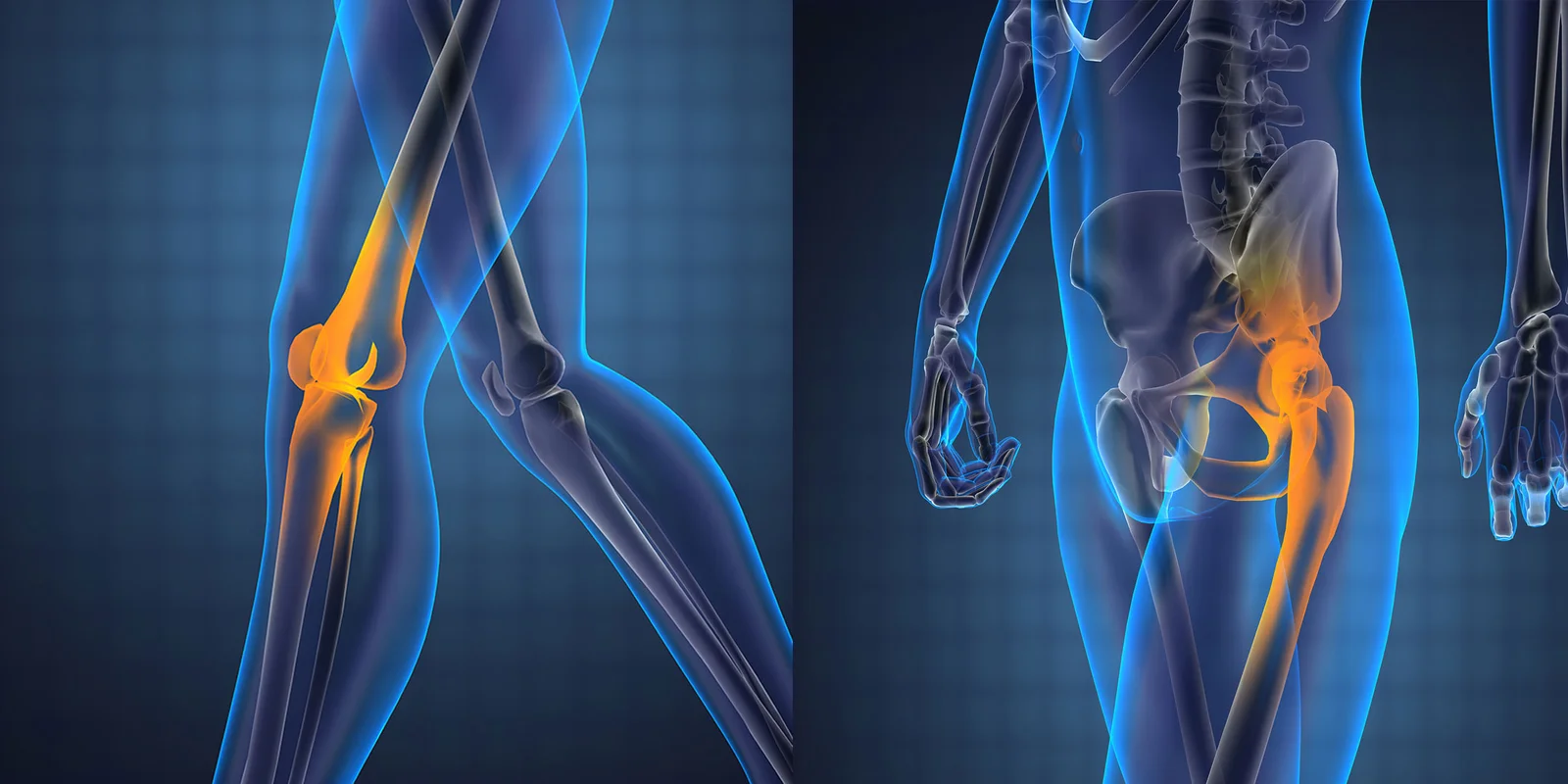
Hip and knee pain are among the most common reasons people seek medical care — particularly as they get older. But knowing when to see a specialist, and what that actually means for treatment, isn’t always clear.
As Dr Anil Goudar explains, seeing an orthopaedic surgeon doesn’t automatically mean surgery.
“There’s a common misconception that once you see a surgeon, you’re signing up for an operation,” Dr Goudar said.
“In reality, our role is to help patients understand what’s going on and what their options are — surgical and non-surgical.”
When Hip or Knee Pain Should Be Assessed
Many people live with hip or knee pain for years, adapting their lifestyle to avoid discomfort. But persistent pain can gradually limit mobility, independence and quality of life.
Dr Goudar says it’s worth seeking further assessment when:
pain is ongoing or worsening
symptoms interfere with daily activities or sleep
mobility is becoming limited
conservative treatments are no longer helping
“Pain is a signal,” he said.
“If it’s affecting how you live, that’s the right time to get it properly assessed.”
Arthritis Is Common — But Surgery Isn’t Always the First Step
With an ageing population in the Illawarra and South Coast regions, arthritis is one of the most common conditions Dr Goudar sees.
“Arthritis is very common, particularly with age-related wear and tear,” he said.
“But that doesn’t mean surgery is always the answer.”
At Joint Vision, patients are supported through a holistic model of care that often begins with non-surgical options, including:
physiotherapy and exercise-based rehabilitation
imaging-guided injections
pain management strategies
activity modification
“If a simpler option can give someone a few more good years of quality of life, that’s often better than rushing into surgery,” Dr Goudar said.
When Surgery Becomes the Right Option
There are situations where surgery is clearly the most appropriate treatment.
“In cases where the joint is bone-on-bone, or where there’s collapse of the femoral head, such as avascular necrosis, delaying surgery doesn’t help,” Dr Goudar said.
“In those cases, the sooner we intervene, the better the outcome — physically and mentally.”
The decision is based on a combination of:
symptoms and functional limitation
imaging findings
overall health and fitness
personal goals and expectations
A Team-Based Approach to Decision-Making
One of the key differences at Joint Vision is the multidisciplinary model of care.
“For me as a surgeon, it’s reassuring,” Dr Goudar said.
“Patients are supported before and after surgery, and any issues are picked up early.”
This includes close collaboration with:
physiotherapists and exercise physiologists
imaging specialists
pain management teams
nursing and post-operative support
“That integrated approach means patients aren’t navigating the system on their own,” he said.
What Patients Often Worry About — And What Matters More
One of the biggest misconceptions Dr Goudar encounters is age.
“Age is just a number,” he said.
“What matters is the patient’s overall health, not how old they are.”
Younger patients sometimes worry they’re “too young” for joint replacement, while older patients fear they’re “too old”.





Leave a Reply